Blogrige
The Official Baldrige Blog
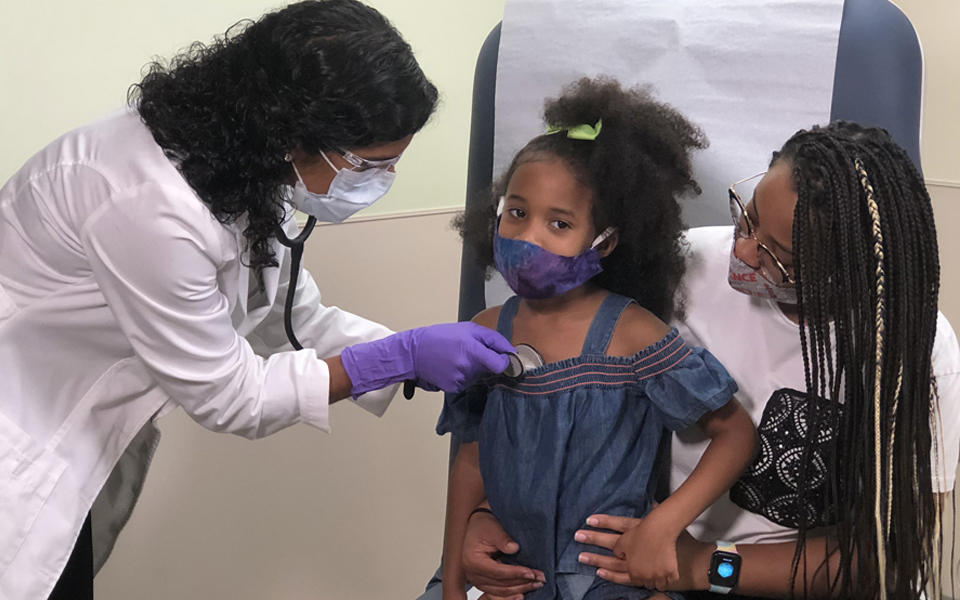

“What would be important to you in the care of your daughter?” John Chessare, president of Baldrige Award recipient GBMC HealthCare, Inc. (GBMC), asked a virtual Quest for Excellence® conference audience.
“The number one answer is always that people want the best possible health outcome for their loved one; but that’s not enough,” he said. “It’s also of the highest importance that we treat our loved ones with compassion and kindness, that we eliminate inordinate waiting and confusion, and we roll all of this into the best possible satisfaction with the way the care is delivered.”
This concept is integrated in GBMC’s memorized vision: "To every patient, every time, we will provide the care that we would want for our own loved ones."

GBMC comprises three integrated work systems: Greater Baltimore Medical
Center, a 257-bed nonprofit, community hospital; GBMC Health Partners, an employed physician group of 300+ primary care providers and specialists; and Gilchrist, an advanced disease, elder, and end-of-life care system.
To support this vision and its four aims, GBMC has defined an integrated leadership system focused on action, redesigned care to focus on patient relationships, and used its health needs assessment to understand community needs.
Importance of Systems and Integration
On the importance of systems, Chessare said,
We have learned through the use of the Baldrige Criteria [the necessity of] implementing a formal leadership system . . . a game plan. It is a system to keep leaders and their teams in action towards our vision.
Chessare added, “When people talk about leadership, most discussions begin and end with personal traits. These personal traits are important, but most organizations . . . implement little measurable change that generates results. And why is this? It’s because leaders get caught in firefighting the issue of the day and push improvement to the back burner.”
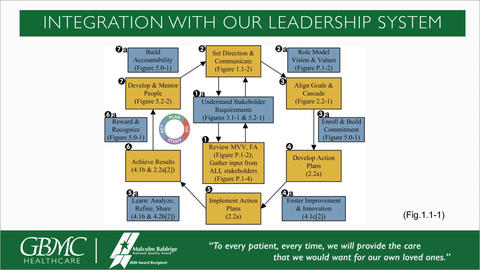
Through study of the Baldrige Criteria, Chessare said GBMC also learned the importance of integration. “We find that . . . integration [of the leadership system] with the performance management system and the performance review process move the leadership system forward faster and help us move closer to our vision at a much greater speed,” he said, adding that the performance review process has daily, monthly, quarterly, and annual check-backs and these include celebrating successes and reviewing areas that need work.
Community Health Needs
To ensure that it understands the health issues facing the people it serves, GBMC conducts a community health needs assessment (CHNA) as part of a community support system, said Chessare. Such an organized system has allowed GBMC to leverage internal and external resources.
Cathy Hamel, president of the Gilchrist work system, said
A pivotal point for her in using the Baldrige Criteria was when GBMC integrated the CHNA and the strategic planning process (SPP). That allows “community needs [to] guide and drive the programs and services offered . . . [and] allows all of the leaders in the organization to fully understand the needs of our community,” she said.
According to Hamel, prior to 2017, the CHNA was driven by the finance team, but today it is driven by population health leaders, which helps GBMC identify and eliminate service gaps. As part of GBMC’s Baldrige journey, it gathered feedback and paused to develop its community benefit system; CHNAs are now used to determine unmet community needs. As service areas grow, GBMC redefines its key communities and broadens the assessment, with findings reported to the annual SPP.
Another important tenet of the Baldrige work is a commitment to continuously improving work through cycles of learning, Hamel said, so in 2021, GBMC integrated its CHNA results with its patients’ self-reported social determinants of health: food insecurity, financial insecurity, and housing.
Core Competency: Redesigning Care
Chessare said that GBMC owes a lot of its success to its core competency of redesigning care, which meant moving from typical primary care to establishing accredited medical homes to ensuring coordinated care and accountability for health outcomes. GBMC chose the patient-centered medical home model to better manage chronic disease.
“With advanced primary care, the concept is not about the visit, it’s about the relationship,” Chessare said. “Once you sign up with one of our patient-centered medical homes, our commitment is that we will be accountable for your health with you.”

He said that GBMC has spent the last decade creating a patient-centered care infrastructure and expanding the services of its health partners to meet the needs of every patient, even those without insurance.
As an example, GBMC opened its first Baltimore city advanced care practice at the Helping Up mission, a residential facility for substance abuse. Before GBMC, the patients were being treated for their addiction, but there was no accountable primary care. GBMC Health Partners is now caring for up to 500 mission clients and 1,500 of its graduates, whom it is supporting in recovery.
In another example of redesigned care, he said, GBMC found out that families were calling 911 because they couldn’t physically transport their loves ones to the physician's office. GBMC has now expanded to serve surrounding neighborhoods, so residents can access care close to home and build relationships with the care team, said Chessare.
As yet another example, through its core competency, GBMC designed a system where it could provide primary care to elders in their own homes through Gilchrist, the largest hospice in Maryland. GBMC is especially proud of Gilchrist, he said, because it is allowing people to live their last days in as much comfort as possible surrounded by their loved ones.

Baldrige Excellence Framework
The Baldrige Excellence Framework has empowered organizations to accomplish their missions, improve results, and become more competitive. It includes the Criteria for Performance Excellence, core values and concepts, and guidelines for evaluating your processes and results.
Purchase your copy today!
Available versions: Business/Nonprofit, Education, and Health Care





