Blogrige
The Official Baldrige Blog
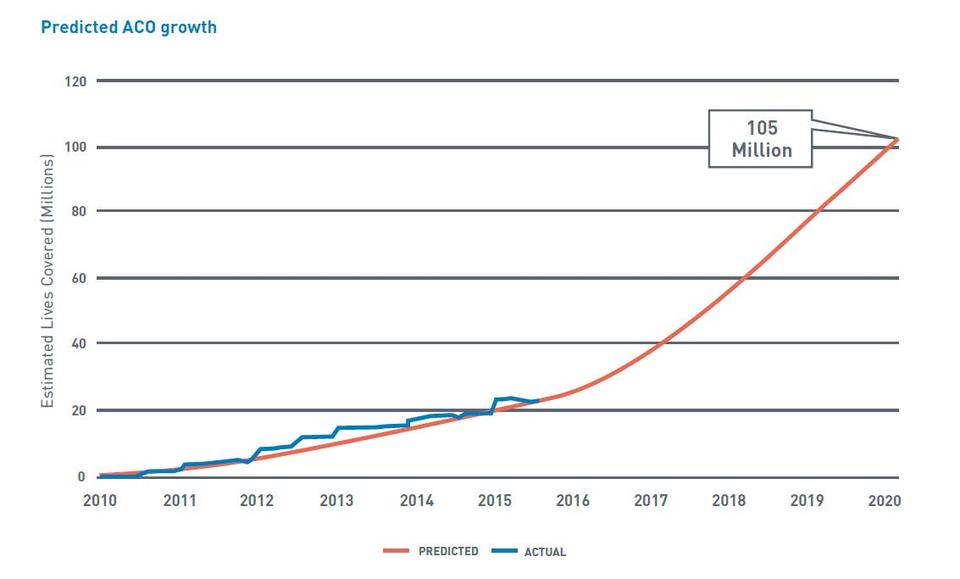
A recent paper “Realizing the Promise: Overcoming the Barriers to ACO Success” explores the promises, doubts, hopes, and future of accountable care organizations (ACOs), with the caveat “it is imperative that you proactively position your organization to take advantage of this opportunity. . . . The number of lives covered through ACOs is anticipated to grow exponentially, reaching more than 105 million patients by 2020, compared to just over 20 million today.”
But me being a staff member of the Baldrige Performance Excellence Program, I was struck by this quote, “The success of any ACO really comes down to the culture. Creating an environment that encourages effective behavior and best practices happens through open, transparent, and passionate leadership.”
While the work of creating and sustaining an ACO seems daunting, the Baldrige Excellence Framework (Health Care) can help—with redefining a culture, creating an environment for effective leadership and behavior, and sharing best practices. The bottom line, Baldrige resources support and enable high-performing ACOs. For example, category 1 of the Criteria (within the framework) provides all of the considerations that leaders need for creating a successful organization now and in the future: an environment for the achievement of your mission, improvement of organizational performance, transparency, organizational learning, and learning for people in the workforce. The Criteria also include considerations for creating a workforce culture that fosters customer engagement, an environment for innovation, and a culture for patient safety.
According to the white paper, “ACOs brought to reality by the Affordable Care Act were designed with a promise: by banding together, physician organizations, hospitals, and other care delivery organizations could share risk, reduce costs, and deliver better holistic care to their patient populations. For a vast majority of ACOs, however, those shared savings have yet to materialize—leaving many doubting that this program solves health care challenges around care coordination and sustainability. There’s still hope, however, for the success of ACOs. Their structural ability to deliver on the tenets of the triple aim— improve the patient experience of care, improve population health, and reduce costs —is strong.”
The white paper lays out four critical barriers to success:
- Effectively lowering costs. According to the white paper, part of this is looking at "cost and utilization metrics to reduce overall spend while maintaining, or improving, quality, as well as having the right clinical decision support tools available to use in maximizing the efficiency of your workflow." In the Criteria, category 4 guides a health care organization in measuring, analyzing, and then improving organizational performance, as well as managing organizational knowledge assets, information, and information technology infrastructure. The Criteria do not prescribe which “clinical decision support tools” an organization should use but provide a framework to guide an organization as to which tools make the most sense and where to use the tools.
- Dealing with shortages of expertise. "Creating an environment that attracts primary care physicians and specialists will be a key determinant between success and failure for any ACO," says the white paper; however, the industry will face a shortage of 46,000 to 90,000 physicians by 2025. In the Baldrige Criteria, physicians are not only critical members of the workforce but in health care organizations with separate administrative/operational and health care provider leaders, “senior leaders” refers to both sets of leaders and the relationship between them. Category 5, Workforce Focus, pays particular attention to recruiting and retaining clinical staff, and physicians are so important to the success of a health care organization that just about every health care Baldrige Award recipient outlines best practices for engaging physicians in their application summaries.
- Creating a successful patient engagement strategy. According to Gene O’Dell, vice president of AHA, “Consumer-driven health care is becoming more relevant and driving new models of care delivery. Now, more than ever, consumers are looking to their own health and developing a trusted partnership with their doctors in medical decisions.” An entire section of the Criteria, 3.2, is dedicated to how to engage patients and other customers by serving their needs and building relationships. Strategy is covered in category 2 and throughout the Criteria, and again this concept is so important that best practices for patient engagement are almost always covered during Baldrige Quest for Excellence® and Regional conferences and in Baldrige Award application summaries.
- Getting the most out of the EMR. "Optimizing an effective system that aggregates clinical, financial, and patient satisfaction data to help hospitals is fundamentally important to allow hospitals to better understand their business," according to the white paper. In the Criteria, considerations for electronic data and health records are laid out in 4.2, Data, Information, and Information Technology, as well as in other areas of the Criteria, including categories for Leadership and Strategy.
For an ACO to succeed, according to the white paper, organizations need to improve the patient experience of care, improve population health, reduce costs, integrate physicians, and ensure that every member of their team understands (or at least appreciates) the importance of quality data (and how they should be gathered, normalized, and made actionable).
I might add one more: implement the Baldrige framework as a roadmap to ensure that you are considering all of these elements to succeed as an ACO. Also, apply for a Baldrige Award so that you can receive objective feedback from Baldrige Examiners on how you are doing to achieve your goals.
What other elements of the Criteria do you think could help health care organizations succeed as ACOs?





