Blogrige
The Official Baldrige Blog


Baldrige Executive Fellow, 2018
David Zaas, MD, MBA, President of Duke Raleigh Hospital, and his organization were already on a journey when he entered the Baldrige Executive Fellows Program. In alignment with Duke Health’s values of excellence in quality and safety, Duke Raleigh Hospital wanted to ensure that zero patients or team members suffered harm while receiving or providing care, acknowledging that a single harm to any patient or team member is one too many. As he entered the Fellows program, his commit-to-zero harm goal became his capstone project, and he was able to use all of the aspects of the fellowship to move toward this goal.
In the following interview, I sought more detail on his capstone project, his experience with the Baldrige Executive Fellows, and the results achieved by Duke Raleigh Hospital, which served more than 69,000 inpatients and 2.3 million outpatients in fiscal year 2018. It offers the Duke Raleigh Cancer Center, Duke Raleigh Orthopaedic and Spine Center, cardiovascular services, neurosciences, advanced digestive care, disease management and prevention, wound healing, outpatient imaging, intensive and progressive care, pain clinic, same-day surgery, emergency department, and community outreach and education programs.
What inspired your capstone project for the Baldrige Executive Fellows?
My capstone project was focused on a journey that I think many health care programs are on: how do we really focus on zero harm to patients and zero harm to each other. We were just starting that journey at the time I knew I would be starting the Baldrige Executive Fellows program. I tried to link my Fellows capstone project to what is a major priority for the organization.
What was the desired goal of your capstone project?
One goal was to empower our team to achieve zero harm for patients and each other. How do we redesign our system in order to empower others to achieve higher reliability, and stay true to safety for patients and each other? Zero harm is so critical in health care.
What results have you seen?
Our team is connected, on a more human level, to each harm at our hospital. Our experiment was simple. We helped people see problems. We wanted to create the ability to see harm to patients and each other in real time and measure it in terms of people impacted. We walked away from statistics and benchmarks and scorecards and focused on identifying harms, learning from them, and sharing what we learned to improve our processes and keep others safe.

How did you help staff to be engaged?
We focused on a new concept for us: how do we use visual management to engage our team? We asked every unit to huddle every day to review our six priority harms to understand every time that we didn’t reach perfect what happened and what we could do differently. I think the key to engaging the team was the use of visual management and the ability to translate this to a human story. The teams on the floor not only knew about a patient or an employee who was harmed but they knew their story. They knew their name. That made it real and I think really motivated them to [think] how do I get to zero next time.
How would you define visual management?
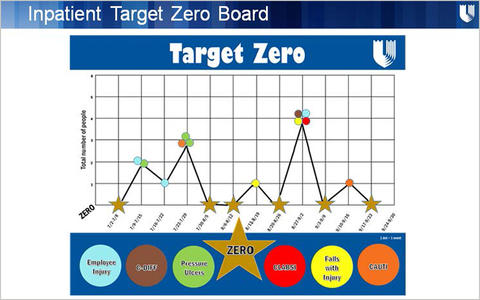
We designed target-zero boards that were put up on every inpatient unit—visible to patients, visible to staff—where we huddled and measured every week the number of harms to patients or staff. We were visibly able to show and talk about each harm every time that we didn’t achieve our goal of zero.
What are the future milestones of your project (i.e., what do you hope will happen next)?
We have already started taking it to the next level. We realized the power in stories and the power of real-time feedback. We’ve gone from talking about the harms weekly to seven days a week. This has given our staff the tools and data to learn to solve problems at their roots. We have also looked at how our leaders can coach our staff to not only see, but share and solve problems better.
We have started to spread our process to other areas of our delivery system. For example, patient harm may be different in the operating room or in a clinic, but we should have that same focus to eliminate harm to patients or team members everywhere that we provide care. We’ve worked with other entities to determine how do we define harm in different care settings. Settings may be very different, but the goal should be the same zero harm.
How have you/your organization continued to use Baldrige resources, including the Baldrige Excellence Framework?
I think the Baldrige framework has been critical. It has helped us identify and frame problems, and gave us tools to evaluate our own leadership and interventions.
We didn’t use the word Baldrige, but we used all of the concepts of the framework. I think the framework will be especially helpful as we continue to grow our problem-solving and sharing techniques.
What was the value for you in completing the Baldrige Executive Fellows Program?
I think the instructors as well as the organizations we visited were unbelievable in terms of their abilities to teach through real examples. They used their experiences to show what many different types of organizations can achieve using the Baldrige framework.
The other part of the fellowship that I thought was really valuable was the opportunity to interact with people who are outside of health care, and to learn and network with them and listen to their different perspectives. We tend to stay within the silos of our industries, but we learned a lot from each other.
Join a Community of Visionary Leaders

Become a Baldrige Executive Fellow
The Baldrige Executive Fellows Program is a hands-on leadership development program that will propel your organization to higher levels of performance. Learn from a cohort of senior decision makers and Baldrige Award recipients and emerge with a broader perspective on how to achieve performance excellence for your organization, stimulate innovation, and build the knowledge and capabilities necessary for organizational sustainability.
What Executive Fellows Are Saying | Apply Today (2020–2021 cohort)





