Summary
Protein-based drugs can degrade by aggregation into micrometer-sized particles. Such particles, although only a minute fraction of the total protein, sometimes stimulate undesirable immune responses. Accurate measurements of particle size and count is needed to understand the role of these particles and support effective regulation, but different measuring techniques can give particle counts that disagree by a factor of ten. We are developing methods for standardizing the response of different instruments. The instability of protein particles precludes their use as a reference material. As an alternative, we have designed and fabricating polymer particles that mimic the properties of protein particles. In another approach, we are developing instrument models that can correct instrumental biases.
Description
Intended Impact
This work will enable industry to obtain accurate, reproducible counts of protein particles, and to differentiate protein particles from other particle types, resulting in greater drug efficacy and safety.
Objectives
- Create a polydisperse suspension of polymer particles that mimic the optical properties of aggregated proteins in solution, over the size range 1 µm to 25 µm.
- Create polymer particles of a well-defined, non-spherical geometry to understand how instrument response varies with deviations from sphericity.
- Develop models for the optical response of particle counting instruments based on both light scattering and optical imaging.
Technical Approach
In the area of instrument models, we are developing mathematical models of the instrument response of a variety of optical particle counting instruments. To model the light scattering process used in light obscuration counters, we treat the protein particles as randomly oriented spheroids with an effective refractive index, and determine the scattering intensity from theory. The finite detection aperture of the light obscuration counter and the small refractive index difference between the particle and the matrix liquid are two critical parameters in these calculations.
In the area of reference materials, we are developing a reference material consisting of a polydisperse distribution of abraded ethylene-tetrafluoroethylene (ETFE) particles. ETFE has several desirable properties: it is chemically inert and very rugged, and has a refractive index close to that of amorphous protein. When abraded, the morphology of the resulting particles closely mimics that of typical protein particles. We are focusing on creating a reference material with effective diameters certified over a range from 0.5 µm to 30 µm. Use of this standard will provide a means of quantifying the instrument response for particles of both low optical contrast and irregular morphology.
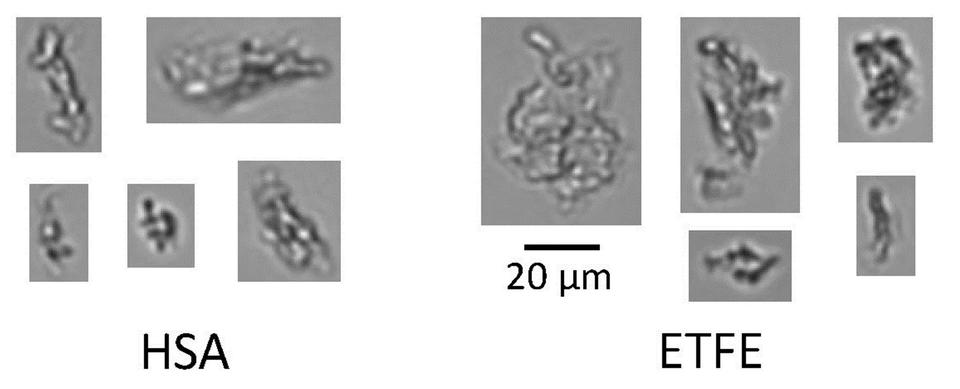
Caption: Aggregates of human serum albumin (HSA, left) and candidate reference material fabricated from ethylene-tetrafluoroethylene (ETFE, right), illustrating the similarities of ETFE particles with protein aggregates.
An alternative method of creating particles with better defined geometry is to use lithographic techniques, in which polymer particles of prescribed geometry are formed on a silicon wafer and then released from the wafer by dissolving a release layer. We have fabricated a range of particles as long as 300 µm and as small as 40 µm long rods with a 2.5 µm x 2.5 µm square cross section. The large particles may be useful as a standard for the counting of visible particles. When released from the silicon wafer, large planar SU-8 particles are flexible and take on three-dimensional shapes. Although all injectable drugs require visual inspection, at present there are no standards available for visible-size particles (diameters greater than approximately 70 µm) that mimic protein particles. Smaller size particles are useful to study the response of instruments to non-spherical particles. Lithographic particles are highly reproducible; however, the refractive index of common photoresist polymers is too high to truly mimic the low optical contrast of typical protein particles. We are engaged in the development of rugged particles with reduced optical contrast.
Major Accomplishments
- Candidate polymer reference material identified that mimics both morphology and optical contrast of protein aggregates
- Measurement and analysis completed for round-robin comparison of candidate reference material, with 24 participating laboratories.
- A variety of lithographic, non-spherical particles fabricated and distributed to industry for evaluation
- Model developed for understanding source of biases for light obscuration particle counters.

