
High-magnification scanning electron microscopy shows (center of micrograph) the leg of an osteoblast (bone precursor), called a cytoplasmic extension, attaching to nano-sized hydroxyapatite crystals, similar to those in natural bone, that make up a CPC implant.
Researchers from the American Dental Association Foundation (ADAF) and the National Institute of Standards and Technology (NIST) have developed a new method for layering two kinds of biomaterials into one strong, yet porous unit that may lead to improved reconstruction or repair of bones.
Currently, calcium phosphate cements (CPCs)—water-based pastes of powdered calcium and a phosphate compound that form hydroxyapatite, a material found in natural bone—are used for reconstructing or repairing skeletal defects, but only in bones that are not load-bearing (such as those in the face and skull). Macropores built into the CPCs make it easier for new bone cells to infuse and, eventually, solidify the implant. Until this happens, however, the macropores leave the implant brittle and susceptible to failure.
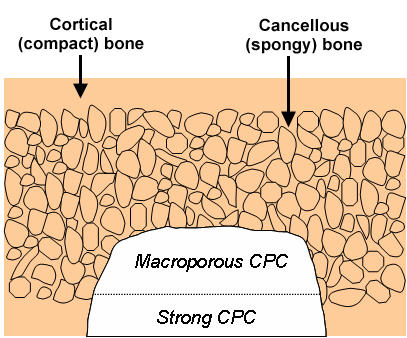
In the September 2007 issue of Biomaterials,* Hockin Xu and colleagues describe a unique approach for providing the strength needed to help an implant better survive its early stages. First, a macroporous CPC paste is placed into the area needing reconstruction or repair. Then, a strong, fiber-reinforced CPC paste is layered onto the first CPC to support the new implant. Once new bone has grown into the macroporous layer and increased its strength, the absorbable fibers in the strong layer dissolve and create additional macroporous channels that promote even more bone tissue ingrowth. This method mimics the natural bone structure in which a strong layer, called cortical bone, covers and strengthens a weaker, macroporous layer (spongy bone).
The two pastes used in the layered CPC method harden in the bone cavity to form an implant that for the first time has both the porosity needed for bone growth and the integrity required for reconstruction or repair of load-bearing bones (such as jaws).
NIST and the ADAF have conducted cooperative research on dental and medical materials since 1928. ADAF researchers focus on development of new dental and biomedical materials, while NIST specializes in the development of improved technologies and methods for measuring materials properties.
The research was funded by the U.S. Public Health Service, NIST and ADAF.
H.K. Xu, E.F. Burguera and L.E. Carey. Strong, macroporous, and in situ-setting calcium phosphate cement-layered structures. Biomaterials 28 (September 2007), pp. 3786-3796.

