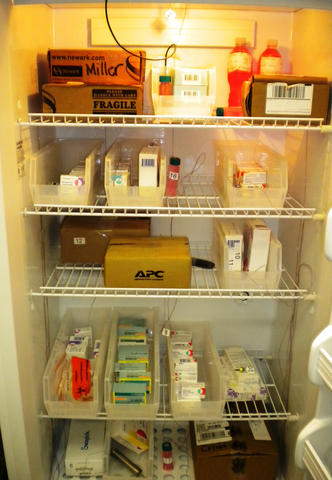
According to a NIST study, vaccines that have not been removed from their packaging (most often a cardboard box), retain their temperature longer than those that have been unpacked and placed in trays. Moreover, the standard-sized refrigerators ability to maintain proper temperature was unaffected by how much vaccine the researchers stored in the refrigerator, a characteristic that was not shared by the dormitory style refrigerators.
Every year, billions of dollars worth of vaccines are shipped to thousands of medical providers across the country, and every year doctors must dispose of tens of millions of dollars worth of those vaccines because they became too warm or too cold while in storage. Now, researchers at the National Institute of Standards and Technology (NIST), with funding from and in collaboration with the Centers for Disease Control and Prevention (CDC), have completed the first of a series of tests to determine best practices for properly storing and monitoring the temperature of refrigerated vaccines.
To ensure they are effective, most vaccines must be kept between 2 and 8 degrees Celsius from the time they are manufactured until they are administered. In addition to the cost of spoiled vaccines that must be destroyed, lack of temperature control probably has resulted in the administering of ineffective vaccinations to the public in a small, but significant, percentage of cases.
In this first phase of a larger study, NIST researchers compared standard-sized refrigerators without freezers against smaller, dormitory-style refrigerators under a variety of conditions, storage practices and use scenarios, including leaving the refrigerator door ajar for various periods, power loss and raising the ambient temperature of the room.
The NIST Thermometry group found that standard-sized, freezerless refrigerators outperformed the smaller, dormitory refrigerators by every measure, but the study also identified several good practices for vaccine storage. Among other things, the group determined that vaccines should never be kept on the door shelves because the relative lack of insulation in the door allowed unacceptable temperature drifts. Vaccines also should be kept away from the walls of the refrigerator, because the defrost cycle can cause the temperature of the walls to shift, and out of the crispers usually found at the very bottom of standard refrigerators because these areas were often shown to drop below 2 degrees Celsius.
In addition, they found that water bottles kept on the door shelves provided thermal ballast which helps to mitigate temperature rises caused by power failure, leaving the door ajar or raising the temperature of the room where the refrigerator is kept.
"While we don't advocate any particular brand of refrigerator, we can say that the standard-sized freezerless refrigerators perform very well, but the dorm-style refrigerators do not and should not be used for storing vaccines," says NIST physicist Gregory Strouse. "Among the many recommendations that we have made, we think one of the most positive upshots of this research is that medical clinics in most cases need not spend several thousand dollars on a pharmaceutical grade refrigerator simply for the purpose of storing vaccines."
The NIST group plans to do further comparisons of standard-sized refrigerators with freezers and pharmaceutical grade refrigerators and begin evaluations of strategies for transporting vaccines overland. They also intend to study various styles of temperature sensors for use in shipping.
Edited on Aug. 25, 2010, to delete an inaccurate reference to possible future activities.
M. Chojnacky, W. Miller, D. Ripple and G. Strouse. Thermal Analysis of Refrigeration Systems Used for Vaccine Storage (NISTIR 7656). November 2009.

