The HoC promises to replace animal testing, shorten drug development timelines and reduce costs. It mimics the interactions of cells within the heart on a small chip and is part of the larger organ-on-a-chip (OoC) suite.
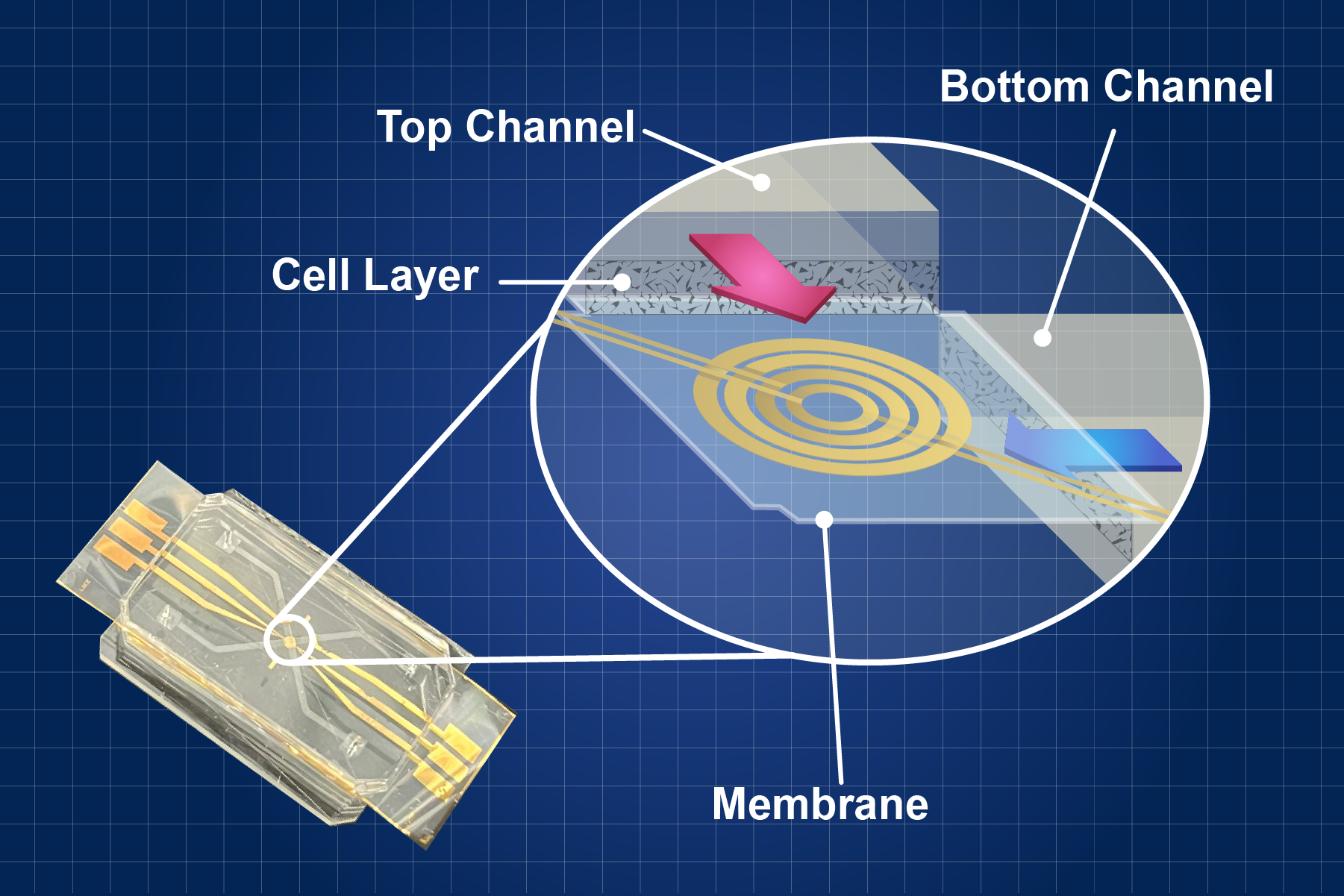
The actual design of the HoC varies, but it is typically a small, transparent or semi-transparent chip consisting of a network of microchannels printed on a layer of polymer.
These microchannels are designed to imitate the blood vessels found in the human heart.
Researchers place human heart cells within these microchannels to manipulate and observe their behavior. Researchers can independently stimulate them or observe their behavior under different conditions, such as the introduction of a drug.

“The heart-on-a-chip is designed to mimic the conditions of a real heart,” says NIST researcher Darwin Reyes, who led the development of this HoC system. “We can manipulate the environment to change stem cells into heart cells and make them contract and relax, as they do in a body to produce a heartbeat.”
The “heart” of the OoC system lies in microfluidics which researchers can use to create advanced models of organs and tissues on small chips in the lab.
“The chip itself can be used with many different cell types,” said Reyes. “In this project in particular, we’re using heart cells, but you can use a customized version of the system with other cells to monitor their behavior visually and electronically.”
The concept of OoC extends beyond the heart. Researchers can create chips that mimic the conditions of various organs, and these chips can even be interconnected to form a multi-organ system.
For example, you could have an HoC connected to a liver-on-a-chip to simulate how the heart and liver interact in response to certain drugs or medical conditions. This approach provides a more comprehensive understanding of how different organs function together in the human body.
In traditional drug development, animals are often used as test subjects. However, animal physiology does not perfectly match human physiology. A drug may pass a test on an animal subject but may then fail in human testing. This not only delays the drug testing process but also puts human test subjects at risk of adverse effects from the drug.
“The ultimate goal is to, if possible, be able to skip the animal testing altogether,” said Reyes. “This would also shorten the time it takes to test drugs, which would hopefully make the medications cost less.”
While HoC is focused on cardiovascular drug development, the OoC capabilities extend beyond a specific organ. The system can be applied to various cell types, including those relevant to cancer research.
“We are in the test phase of understanding how we can track the movement and aggressiveness of cancer cells in real time,” says Reyes,“Our hope is, in the future, with more testing, the system may be able to provide measurements of cancer cell aggressiveness that could help with diagnosis.”
 Electronics Weekly Electronics Design & Components Tech News
Electronics Weekly Electronics Design & Components Tech News



